Types of Skin Cancer
Basal Cell Carcinoma (BCC)
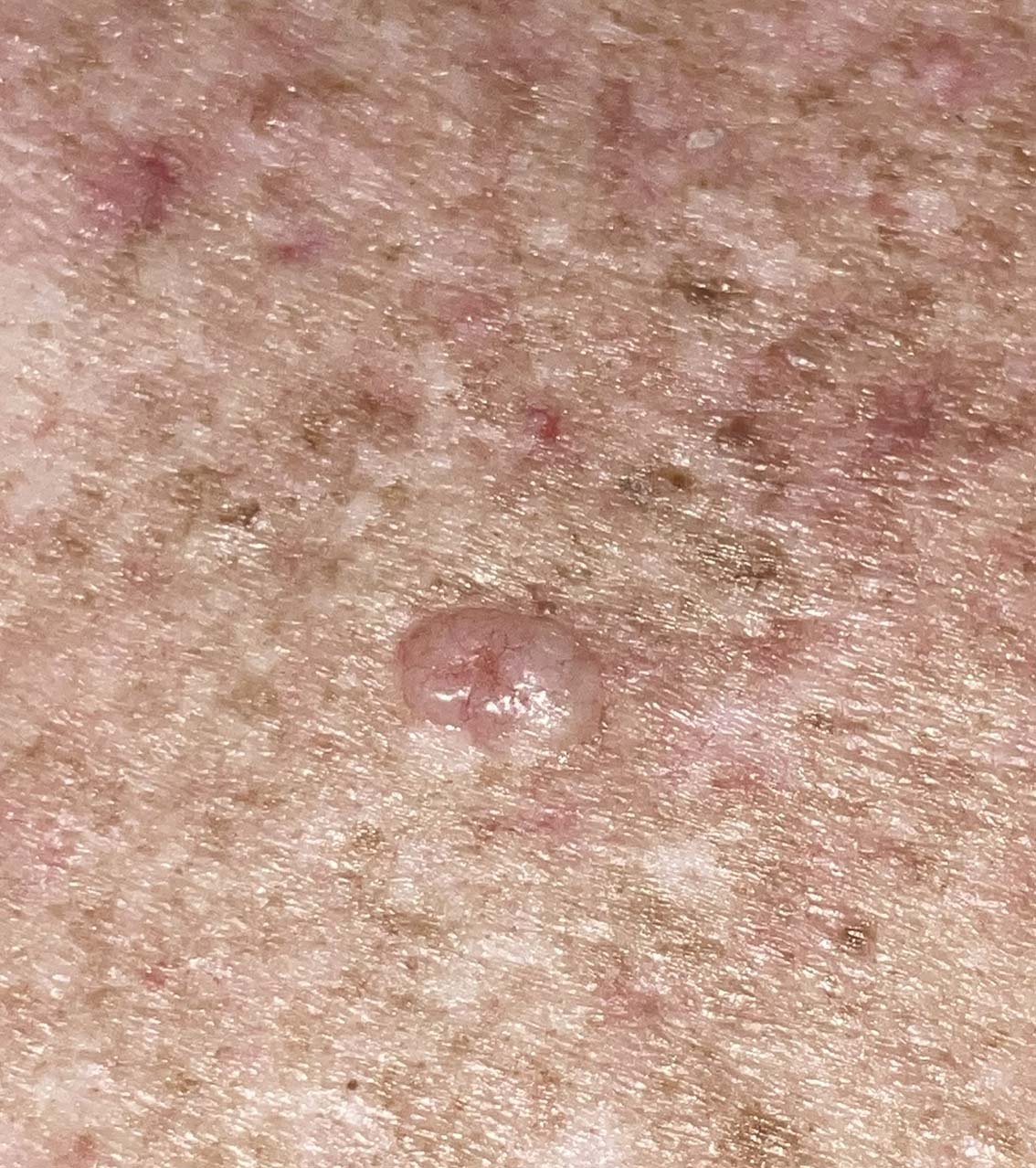
Basal Cell Carcinoma (BCC) is the most common skin cancer in Australia and accounts for 2/3rds of all skin cancers. It is a tumour of the basement cells in the outermost layer of the skin. It rarely metastasizes to other parts of the body but can cause local destruction of tissues. The most common sub type is a nodular BCC and this presents as a small pearly pink nodule. Other subtypes can be flat pink lesions that look different to the surrounding skin. “Towelling” is when a lesion bleeds with minimal trauma like wiping a towel over your nose. This is highly suspicious for BCC. If a spot doesn’t go away for 8 weeks it needs to be reviewed by a skin cancer doctor. Early identification of BCCs enables less aggressive treatment options.
Basal cell carcinoma through a dermatoscope.
Basal cell carcinoma to the naked eye.
Squamous Cell Carcinoma (SCC)
Squamous Cell Carcinoma (SCC) accounts for almost 1/3 of skin cancers and much more common on chronically sun exposed skin such as the head, neck and legs. SCC’s have much greater capacity to metastasize to the lymph nodes and distant sites. The most common sites for metastases are the lip, the ear and the nose. If you develop a tender lump or open sore that wont heal it should be checked immediately. Subtypes of SCCs can grow rapidly and double in size in 2 weeks.
As our immune system dampens in older age these skin cancers become much more prevalent. Similarly any immunosuppression is a significant risk factor for SCCs. Anyone who has been on immunosuppressants, had chemotherapy for other cancers or has had an organ transplant should have regular skin checks.
While overwhelmingly the major cause for SCCs is UV damage from the sun, other causes include burns, radiotherapy and solarium bed use (12 fold increase if used for 2 years).
Most SCCs originate from patches of early damage to the superficial skin called solar keratosis. A more aggressive approach to treat them at this early stage is often warranted in chronically sun damaged Australian skin. Options include Topical cream treatment and Photodynamic Therapy.
A famous Australian study called the Nambour trial, showed a significant reduction in SCC formation in people who applied daily sunscreen. This is the most important photoageing and skin cancer regime you can do for your skin.
https://www.science.org.au/curious/people-medicine/study-saved-our-skin
Melanoma
Melanoma of the skin is the most common cancer in Australians aged 20-39.
On average, 16,000 Melanomas will be diagnosed in Australia and 1300 Australians will die from Melanoma each year. That’s a death from Melanoma every 6 hours!
If identified early in the first layer of skin and treated appropriately, 5 year survival rates are >99%.
Thanks largely to advancement in dermoscopic examination by skin cancer doctors in primary care we are finding early, less advanced Melanoma.
Risk factors for you having a Melanoma are:
History of blistering sunburns, especially at a young age
Fair skin, freckles, blue eyes
Having many moles >100
Having moles that are atypical, or look different from normal moles. There is a genetic condition called Dysplastic Naevus Syndrome which is estimated to increase risk of lifetime melanoma by 7 times.
Family History of Melanoma
Personal history of Melanoma or other skin cancers
Others risks include immunosuppression, being male, previous use of tanning beds and Parkinsons Disease.
Most Melanomas arise from normal skin (70-75%) not from a pre existing mole (25-30%). After the age of 45 you shouldn’t get any new moles and none of your existing moles should change.
<2% of Melanomas are raised, nodular forms. They are only itchy and bleed in advanced disease.
In the early stages, melanomas can look very subtle, and nothing like they do on the posters. This is when it is best to find and treat them. There is great variation in how melanomas look, from a pink patch to a lightly or darkly pigmented spot. The vast majority of melanomas found at our clinic were not previously concerning to the patient.
So, protecting yourself from UV damage, annual skin checks with a well trained skin doctor and regular self checks gives you the best chance to minimise your risk of harm from Melanoma.
Early melanoma in situ changing on short term monitoring with a dermatoscope.
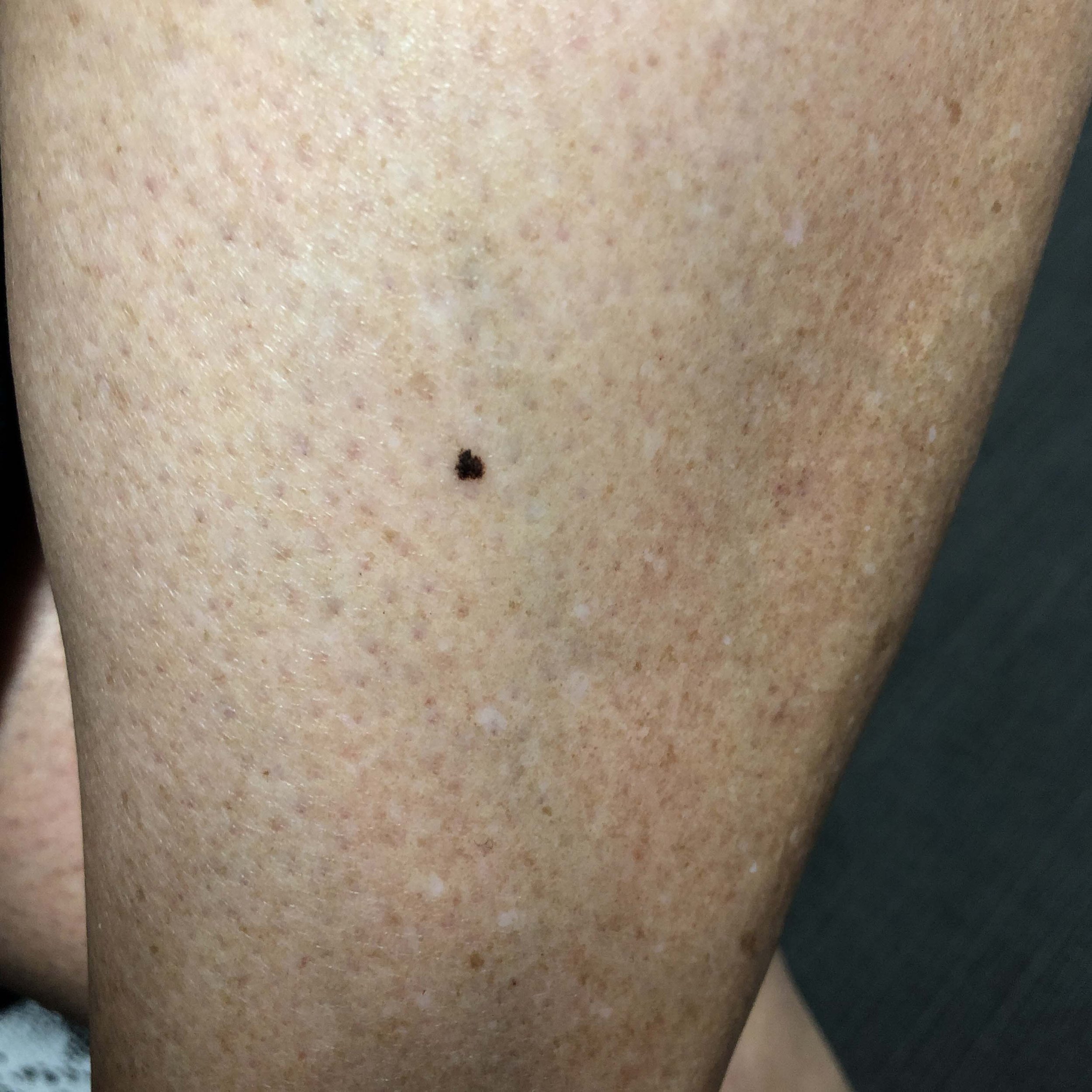
Melanoma clinical imaging.
Melanoma clinical imaging.